If you’ve been battling persistent low back pain with no clear cause, you might be overlooking a crucial piece of the puzzle: your pelvic floor. The short answer is a resounding yes, can pelvic floor dysfunction cause back pain. This connection is one of the most common, yet frequently missed, drivers of chronic lumbar, sacral, and hip pain.
Understanding this link is the first step toward finding lasting relief. Your pelvic floor doesn’t work in isolation; it’s a key player on a team of muscles that stabilize your entire core. When it’s not functioning correctly, your back often pays the price.
What is the Pelvic Floor? A Quick Refresher
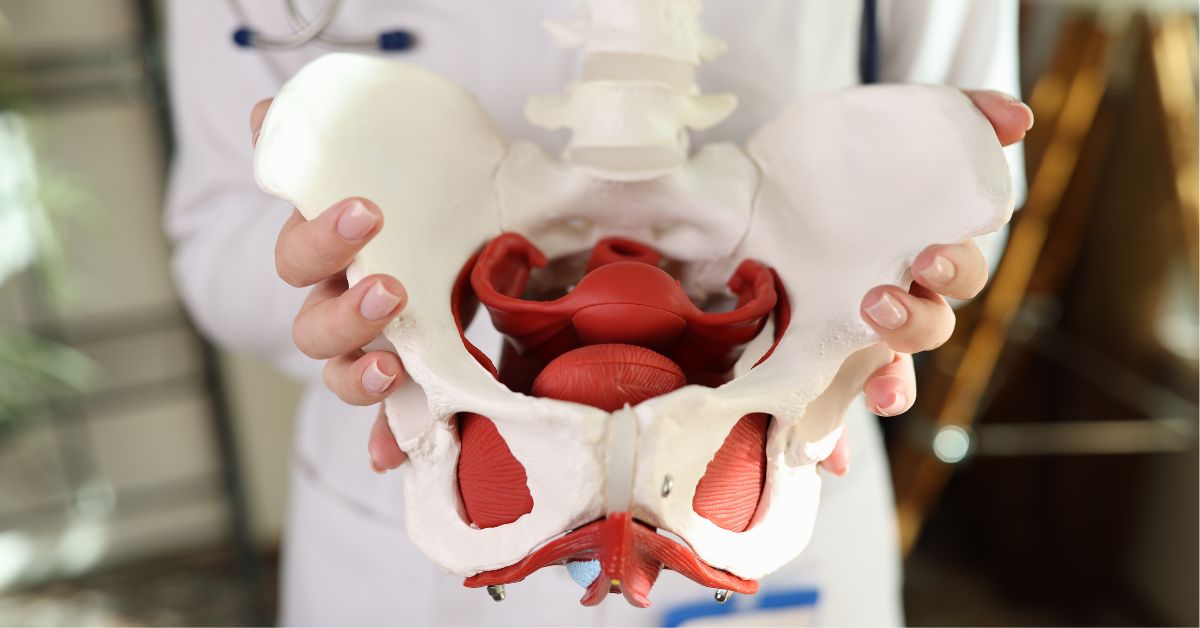
Think of your pelvic floor as a muscular hammock or sling stretching from your pubic bone in the front to your tailbone in the back. This intricate network of muscles, ligaments, and connective tissues has several vital jobs. Its primary functions include:
- Support: It holds up your pelvic organs, including the bladder, uterus (in women), and rectum.
- Stability: It works with your deep abdominal muscles, back muscles, and diaphragm to stabilize your spine and pelvis.
- Control: It helps you control your bladder and bowel function (sphincter function).
- Sexual Function: It plays a role in sexual arousal and orgasm.
Understanding Pelvic Floor Dysfunction (PFD)

Pelvic Floor Dysfunction (PFD) occurs when you’re unable to correctly control the muscles of your pelvic floor. It’s not just about weakness. PFD can manifest in two main ways:
- Hypotonic (Weak): The muscles lack the tension and strength needed to provide adequate support, often leading to conditions such as stress incontinence or pelvic organ prolapse.
- Hypertonic (Tight): The muscles are too tense and are unable to relax properly. This is a very common, yet often undiagnosed, cause of pain.
Because the symptoms can be so varied, PFD is often misdiagnosed. Recognizing the signs is key to getting the right help.
Common Pelvic Floor Dysfunction Symptoms
While back pain is a major indicator, it rarely appears alone. If you have PFD, you might also experience one or more of the following pelvic floor dysfunction symptoms:
- Urinary or fecal incontinence (leaking)
- An urgent or frequent need to urinate
- Painful urination
- Constipation or straining with bowel movements
- Pain during or after sexual intercourse
- Unexplained pain in your genitals, rectum, or pelvis
- A feeling of heaviness or pressure in the pelvis
If any of these sound familiar alongside your back pain, it’s a strong sign that the two could be related.
The Core Canister: How the Back Pain Pelvic Floor Connection Works
To truly understand the back pain pelvic floor connection, you need to think of your core as a “canister” or a pressure-filled cylinder. This canister has four main parts that work together in perfect energy.
- The Top: Your diaphragm (your primary breathing muscle).
- The Bottom: Your pelvic floor muscles.
- The Front & Sides: Your deep abdominal muscles (transverse abdominis).
- The Back: Your deep spinal muscles (multifidus).
When every part of this canister is working well, your spine is supported, pressure is managed, and movement is efficient. However, if the pelvic floor at the bottom of the canister is dysfunctional, the whole system is thrown off balance.
If your pelvic floor is too tight (hypertonic), it can physically pull on your tailbone and sacrum, altering the alignment of your pelvis. This misalignment creates tension and strain on the sacroiliac (SI) joints and lumbar spine, directly causing low back pain. These tight muscles also can’t function properly, creating instability.
If your pelvic floor is too weak (hypotonic), it fails to provide a stable base for your spine. To compensate for this lack of support, your back muscles and hip muscles have to work overtime. This chronic overuse leads to muscle fatigue, tightness, spasms, and persistent pain.
Finding Relief: The Role of Physical Therapy and Pelvic Floor Rehabilitation
The most effective way to address this issue is not with more back stretches or crunches, but with targeted pelvic floor rehabilitation. This is where a specialized physical therapist comes in.
A specialist in women’s health physical therapy or pelvic health (who treats all genders) is trained to diagnose and treat PFD. A typical physical therapy pelvic floor treatment plan is highly individualized and goes far beyond just doing Kegels.
Your therapist will perform a comprehensive evaluation to determine if your muscles are weak, tight, or uncoordinated. Treatment may include:
- Manual Therapy: Hands-on techniques to release tight muscles and trigger points in the pelvic floor, hips, and low back.
- Biofeedback: Using sensors to help you learn how to properly contract and, more importantly, relax your pelvic floor muscles.
- Targeted Exercises: A customized program that may include strengthening for weak muscles or “reverse Kegels” and relaxation techniques for tight muscles.
- Breathing Coordination: Retraining you to use your diaphragm correctly, which is essential for regulating pressure within the core canister and relaxing the pelvic floor.
- Postural Education: Making adjustments to how you sit, stand, and lift to reduce strain on both your back and pelvic floor.
This holistic approach, known as pelvic floor therapy, addresses the root cause of your back pain instead of just chasing the symptoms.
What You Can Do at Home
While waiting for a professional evaluation, there are a few safe things you can do to start easing tension. These techniques focus on relaxation, as many people unknowingly hold tension in their pelvic floor.
1. Diaphragmatic (Belly) Breathing:
Lie on your back with your knees bent. Place one hand on your chest and one on your belly. As you inhale slowly through your nose, let your belly rise, and your pelvic floor gently relax and lower. As you exhale, let your belly fall naturally. The hand on your chest should remain relatively still. This helps coordinate the core system and promotes relaxation.
2. Gentle Stretches:
Stretches like Child’s Pose, Happy Baby, and gentle knee-to-chest hugs can help release tension in the surrounding hip and back muscles, thereby indirectly relaxing the pelvic floor.

Important Note: Avoid doing Kegel exercises without guidance. If your pelvic floor is tight, Kegels can make your pain and symptoms significantly worse by further tightening already tense muscles.
Conclusion: Don’t Ignore the Connection
So, can pelvic floor dysfunction cause back pain? The evidence is clear: it is a significant and often primary cause. Your body is an interconnected system, and the pain you feel in your back may be a distress signal from a dysfunctional pelvic floor.
If you have been struggling with chronic low back pain that defies traditional treatment, it’s time to look deeper. Seeking an evaluation from a pelvic health physical therapist could be the missing link to understanding your pain and finally finding a path to lasting relief.