Many people suffer in silence with issues like bladder leakage when they laugh, persistent pelvic pain, or discomfort after childbirth. They often assume it’s just a normal part of aging or motherhood. But what if there were a specialized, non-surgical treatment designed to address these very problems?
Welcome to the world of pelvic floor therapy. This highly effective form of physical therapy is a game-changer for countless individuals, offering a path to recovery and improved quality of life. This guide will demystify the entire pelvic floor therapy what to expect, so you know exactly what to expect on your journey to better health.
What is the Pelvic Floor and Why Does it Matter?
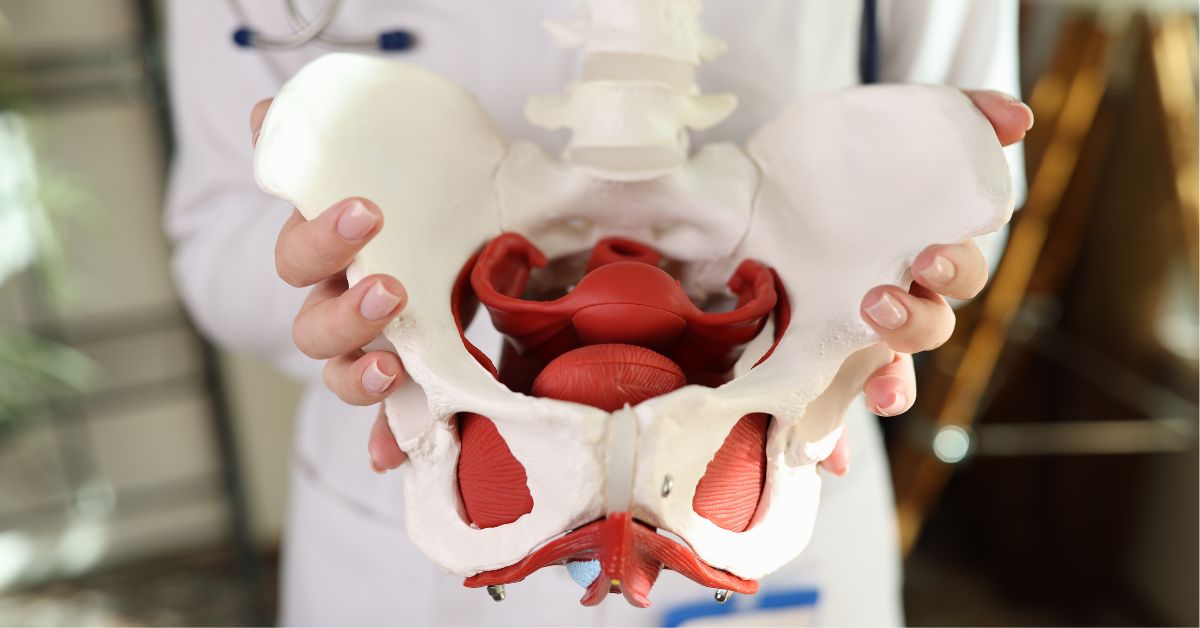
Think of your pelvic floor as a muscular hammock or sling that stretches from your pubic bone in the front to your tailbone in the back. This intricate network of muscles, ligaments, and connective tissues has several vital jobs.
Your pelvic floor is responsible for:
- Support: It holds up your pelvic organs, including the bladder, uterus (in women), and rectum.
- Continence: It controls the sphincters for your bladder and bowels, allowing you to go to the bathroom when you want to.
- Stability: It works with your deep abdominal muscles, back muscles, and diaphragm to stabilize your core.
- Sexual Function: These muscles play a key role in arousal and orgasm.
When these muscles become too weak (hypotonic) or too tight (hypertonic), it can lead to a wide range of problems. This can be caused by pregnancy, childbirth, surgery, chronic coughing, heavy lifting, or even high-impact exercise.
Signs You Might Need Pelvic Floor Physical Therapy
Pelvic floor dysfunction is incredibly common, but it is not normal. If you experience any of the following symptoms, a specialized physical therapist can help create a targeted pelvic rehabilitation plan for you.
- Urinary Issues: Leaking urine when you cough, sneeze, or exercise (stress incontinence), or a sudden, intense urge to urinate (urge incontinence).
- Bowel Problems: Fecal incontinence or chronic constipation and straining.
- Pelvic Pain: Pain in the pelvis, genitals, or rectum. This is a primary focus of pelvic pain treatment.
- Painful Intercourse: Discomfort during or after sexual activity (dyspareunia).
- Pelvic Organ Prolapse: A feeling of heaviness, bulging, or pressure in the pelvis, often described as feeling like “something is falling out.”
- Postpartum Recovery: A core component of postpartum pelvic therapy is addressing issues like diastasis recti (abdominal separation), perineal tearing, and C-section scar recovery.
The Pelvic Floor Therapy Treatment Process: A Step-by-Step Guide
Knowing pelvic floor therapy what to expect can significantly ease any anxiety about your first appointment. The process is professional, confidential, and tailored completely to you.
Step 1: The Initial Consultation & Evaluation
Your first visit is all about understanding you and your unique symptoms. Your therapist will conduct a thorough assessment, which includes a detailed discussion of your medical history, symptoms, and health goals.
The physical evaluation typically involves an external and internal assessment. The external exam looks at your posture, breathing patterns, core strength, and hip mobility. With your explicit consent, an internal exam may be performed to directly assess the strength, tone, and coordination of your pelvic floor muscles. This is the gold standard for an accurate diagnosis, but is always your choice.
Step 2: Your Personalized Treatment Plan
Based on the evaluation, your therapist will develop a personalized treatment plan. There is no one-size-fits-all approach in women’s pelvic health therapy. Your plan will be designed to address your specific muscle imbalances and symptoms.
Step 3: Ongoing Therapy Sessions
Follow-up sessions usually last between 45 and 60 minutes. During these appointments, you will work one-on-one with your therapist to progress through your treatment plan, which may involve a combination of the techniques below. You will also be given a home exercise program to ensure continued progress between visits.
Common Techniques Used in Pelvic Rehabilitation
Your therapist has a variety of tools and techniques to help you heal. Your plan will likely include a combination of the following evidence-based treatments.
Manual Therapy
This involves hands-on techniques in which the therapist uses gentle pressure to stretch and release tight tissues and trigger points in the pelvic floor muscles, abdomen, and surrounding joints. This is crucial for alleviating pain and restoring normal muscle function.
Pelvic Floor Exercises Therapy

This is much more than just “doing Kegels.” While Kegels (strengthening contractions) are important for weak muscles, many people with pelvic pain actually have overly tight muscles and need to learn how to relax them (a “reverse Kegel”). Your therapist will teach you how to correctly isolate, contract, and, just as importantly, relax your pelvic floor muscles in coordination with your breath.
Biofeedback
Biofeedback is a powerful tool that helps you “see” your pelvic floor muscles working in real-time. A small sensor provides visual or auditory feedback on a screen, helping you learn how to properly contract and relax muscles you can’t see. It’s an excellent way to improve muscle awareness and coordination.
Education
A huge part of therapy is learning about your body. Your therapist will educate you on proper bladder and bowel habits, posture modifications, and strategies to manage pressure during daily activities to protect your pelvic floor in the long term.
Key Pelvic Floor Therapy Benefits You Can Experience
Committing to a pelvic therapy program can lead to life-changing results. The ultimate goal is to restore function and get you back to living your life without limitations.
- Improved Bladder and Bowel Control: A primary goal of bladder control therapy is to reduce leakage and urgency.
- Decreased Pelvic Pain: Effectively addresses the root muscular cause of pain during intercourse, sitting, or daily activities.
- Enhanced Core Strength: A functional pelvic floor is the foundation of a strong, stable core.
- Optimal Postpartum Recovery: Helps heal perineal tears, manage C-section scars, and safely return to exercise.
- Improved Sexual Health: Can lead to decreased pain, increased sensation, and stronger orgasms.
- Prevention of Future Problems: Proactively strengthening and coordinating these muscles can help prevent or manage pelvic organ prolapse.
Who Can Benefit from Pelvic Health Therapy?
While often associated with postpartum care, pelvic floor physical therapy benefits a wide range of individuals. This includes:
- Postpartum Women: Essential for anyone who has given birth, whether vaginally or via C-section.
- Athletes: Runners, weightlifters, and gymnasts who experience leakage due to high-impact activity.
- Menopausal and Post-Menopausal Women: To address changes in tissue and muscle tone related to hormonal shifts.
- Individuals with Chronic Pelvic Pain: Those diagnosed with conditions like endometriosis, interstitial cystitis, or pudendal neuralgia.
- Men: Men can also experience pelvic floor dysfunction, especially after prostate surgery or with chronic pelvic pain.
Conclusion: Take the First Step Towards Pelvic Wellness
Pelvic floor dysfunction is common, but it should never be considered a normal or acceptable part of your life. You do not have to “just live with it.” Pelvic floor therapy is a safe, effective, and evidence-based treatment that empowers you to regain control over your body and your health.
If you are experiencing any of the symptoms discussed, the first step is to talk to your doctor or consult a physical therapist specializing in pelvic health. Taking that step is a powerful move towards a more comfortable, confident, and active future.